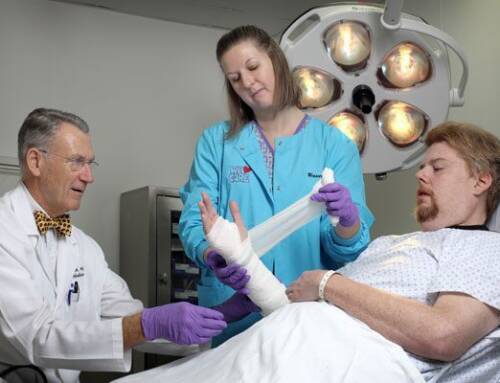
A former volunteer firefighter who sustained burns and partial amputation of his fingers on both hands continues to suffer from PTSD, flashbacks and sleep disturbances. His pain management physician has ordered a genetic study to help understand how he reacts to treatment based on his genetic factors.
Genetic testing in pain management is becoming more prevalent. Just as people have differences in hair color and eye color, people are also different in their responses to pain and to medications. Modern genetic medicine may be a viable way to explain the variability of personal responses to medication and predict more effective medications for patients. In identifying genetic risks and the most effective analgesic for individual patients, clinicians may be able to improve the efficacy of medication and decrease risks posed by medications, such as overdose, addiction and death. Another consideration for bioscience testing is the potential economic feasibility. Using oral samples or swabs could provide a dramatic price decrease for genetic testing.
One doctor provided the following tips to clinicians prescribing medications:
(1) take the medication history of prior adverse or ineffective medication effects;
(2) check for common potential interactions with opioids;
(3) with new medications, check the patient’s metabolic pathway for activation or excretion issues;
(4) be mindful of and evaluate potential interactions between drugs when adding new medications;
(5) consider formal genetic testing to evaluate opioid choices and help predict potential opioid risks.